Pain administration looks deceptively basic from the exterior. Give an analgesic, reassess, discharge. In real practice, it is just one of the most nuanced parts of nursing. Clients show up strained with anxiety, complex comorbidities, polypharmacy, and a history that may consist of opioid dependancy or undertreated discomfort. You handle physiology, law, documents, and human feeling, typically under time pressure. That is the context for PUAEME008, the Australian system of competency that focuses on supplying discomfort relief in emergency and pre-hospital settings. If you are considering pain management training courses, going for a discomfort monitoring certificate, or picking brief courses in pain administration to sharpen your side, it pays to understand what this system covers and just how to turn it into everyday competence.
What PUAEME008 actually implies in practice
PUAEME008 is generally referred to as "Offer discomfort management." In lots of solutions it is a prerequisite to administer particular analgesics under method, specifically inhaled agents and some parenteral options through standing orders. While specific drug scopes vary by jurisdiction and company, the core of PUAEME008 provide pain management is less about the particle and even more regarding risk-free, effective systems:
- Assessment that separates pain as a sign from discomfort as a disorder. An individual with squashing breast pain is not the same as a person with musculoskeletal strain. Risk triage for red flags: shock, neurovascular concession, compartment disorder, sepsis, head injury with deteriorating GCS, and feasible drug-seeking habits that can shadow assessment. Analgesic selection matched to device, seriousness, comorbidities, and atmosphere. The "right medication" relies on whether you have oxygen, monitoring, IV gain access to, and the skills to save the airway. Monitoring and titration to effect, not to habit. Repeat evaluations drive dose decisions and escalation. Documentation that safeguards your medical reasoning and fulfills medicolegal standards.
Successful prospects in a PUAEME008 give discomfort administration training course reveal that they can apply these principles under tension, not simply state them in a classroom.
Where nurses run into PUAEME008
I initially completed the device throughout a change from ward nursing to mixed ED-ambulance work in a rural service. We did not have instant clinical cover after hours. Analgesia choices had consequences, and the local tertiary healthcare facility sat 90 mins away along roads that cold over by twelve o'clock at night. PUAEME008 accredited me to give breathed in methoxyflurane, titrate fentanyl under procedure, and escalate for ketamine with medical consultation. That scope will certainly vary, however the structure really felt universal.
Nurses satisfy this unit in 3 primary contexts:
- Pre-hospital or retrieval environments where standing orders need a proficiency like PUAEME008 to provide analgesia without a prescriber on-site. Emergency departments and urgent treatment centers where nurse-initiated analgesia pathways exist. Remote and country facilities where nurses take care of discomfort throughout long term transportation intervals.
Even if your setup maintains analgesic management purely under clinical orders, the evaluation, tracking, and documents components of the system elevate your practice and minimize medical risk.
Competencies you must demonstrate
A good pain monitoring training course that lines up to PUAEME008 will certainly not be a slideshow of drug facts. Anticipate to show four wide competencies:
Clinical evaluation. You will certainly be expected to make use of a validated pain scale, but extra significantly you will reveal you can determine the most likely pain system from history and exam. That means localizing discomfort, mapping radiation, checking neurovascular status, evaluating for warnings, and determining when analgesia has to wait on life-saving interventions. For example, a hypotensive injury individual may require blood products prior to anything else.
Analgesia choice and dosing. You will certainly validate why a given individual obtains a specific agent, at an offered starting dose, with a mentioned plan to titrate. Combined agents have harmony and trade-offs. For example, matching paracetamol and an NSAID lowers opioid demands in Visit this site several bone and joint injuries, yet NSAIDs are an inadequate selection for presumed crack with bleeding risk or renal disability. In a wheezing individual with severe discomfort, ketamine might be safer than morphine because of its marginal respiratory system depression.
Monitoring and acceleration. The unit anticipates you to look for therapeutic effect and negative effects, to adjust dosage, to switch representatives if required, and to understand when to call for backup. Breathed in analgesia might be enough for a dislocated shoulder reduction, however a femoral shaft crack throughout a lengthy transportation might need IV options and local strategies if available.
Communication and documents. You ought to be able to turn over clearly to paramedics, ED colleagues, or an access team. Great paperwork adheres to the chain: assessment, decision, drug and dose, response, damaging effects, and strategy. It is likewise your shield if a case is reviewed.
Matching program options to your role
The pain management programs market is crowded. Names differ, and not every offering associate PUAEME008. When evaluating companies of pain monitoring training courses, seek these attributes:
- Nationally recognised system mapping that particularly notes PUAEME008 provide pain monitoring, not simply a common "acute pain" module. Practical situations and simulation with skills sign-off, not just e-learning. If your function includes inhaled analgesia or IV titration, you should take care of tools and perform simulated dosing and monitoring. Clear analysis amount of time and re-certification requirements. Analgesia proficiencies generally run out after 1 to 3 years, with updates on protocols and pharmacovigilance. Trainer qualifications with pre-hospital or ED experience. You want educators that have actually made these decisions at 3 a.m., not just in lecture halls.
Short courses in pain management can be beneficial if they enhance the core abilities with hands-on method. A certification training course suffering administration that includes study, pharmacology refreshers, and emergency discomfort monitoring drills has a tendency to have the very best transfer to the floor.
What "excellent" method appears like at the bedside
A new graduate once asked why I spent three added minutes gathering background prior to providing an analgesic to an individual with ankle pain. The reason was straightforward. The ankle was not the issue. The proximal fibula hurt, the foot was cold, and the individual had pain disproportionate to touch. The differential consisted of a vascular concern, and immediate imaging trumped early NSAIDs. A pain monitoring certification need to instruct you to calibrate this sort of judgment.
When analgesia is appropriate, match the medication to the task:
- Mild to modest bone and joint discomfort without red flags frequently responds to paracetamol and an NSAID, plus ice, altitude, and immobilisation. Opioids include little advantage when the basic procedures are neglected. Severe stressful discomfort on scene may ask for inhaled analgesia as a bridge. It buys time to develop IV access, splint appropriately, and plan clear-cut analgesia en route. Renal colic can prefer ketorolac when renal feature enables, with judicious opioid titration if needed. Metoclopramide covers nausea and can aid with opioid sparing. Fracture decrease or misplacement needs planning: appropriate analgesia and muscle mass leisure, surveillance, and post-procedure neurovascular reassessment.
Nurses with PUAEME008 competency are typically the initial to act. The most effective ones do not skip the basics of comfort: repositioning, cozy coverings, peaceful setting. Those information reduced general analgesic requirements, specifically in older adults.
Pharmacology you will in fact use
A pain administration accreditation program hangs around on pharmacology, however remembering medication graphes is not the result. You need fluency with the patterns.
Paracetamol continues to be the most safe very first step in a lot of patients. Dose matters. Grownups normally receive 1 g orally or IV every 6 hours, conscious of collective day-to-day limitations, liver disease, and poor nutrition. It is stackable with nearly everything else.
NSAIDs supply strong alleviation for inflammatory pain: strains, renal colic, oral pain, and post-op discomfort when enabled. They are contraindicated or risky in GI blood loss, advanced kidney problems, improperly regulated cardiac arrest, and late maternity. Courses must cover agent-specific subtleties, like the start and kidney impact of ketorolac versus ibuprofen, and when to avoid them in trauma with possible bleeding.
Opioids are devices, not remedies. Morphine, fentanyl, and oxycodone each have profiles that matter. Morphine brings histamine launch and hypotension threat in some patients. Fentanyl works promptly, which is beneficial in titration, yet it does not last long. Oxycodone is simple to recommend poorly and easy to taper improperly. Respiratory system anxiety is the hazard that gets the headlines, but the more common issues are nausea or vomiting, vomiting, irregular bowel movements, and delirium in older grownups. PUAEME008 training worries titrate-to-effect dosing and strenuous monitoring.
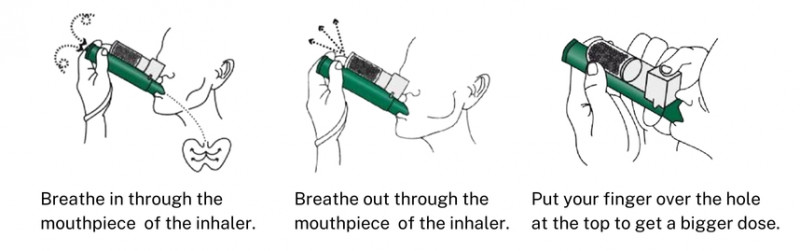
Inhaled analgesia such as methoxyflurane prevails in pre-hospital and minor treatment settings. It is patient-controlled and fast to begin, though restricted by cumulative dose ceilings and possible nephrotoxicity with prolonged or repeated use. You need to recognize how to advise people, make certain appropriate air flow in constrained spaces, and acknowledge when the inhaler masks hypoventilation or hypoxia.
Ketamine has taken a particular niche in emergency situation pain monitoring for severe injury, burns, and opioid-tolerant patients. Sub-dissociative dosing provides analgesia with minimal respiratory system depression, however high blood pressure, tachycardia, and appearance responses can take place. It demands surveillance and training, which numerous pain administration training programs now include.

Regional blocks are significantly component of nurse-led methods in some services, specifically femoral nerve obstructs for hip cracks supervised by sophisticated experts or physicians. If your scope includes this, your certificate program suffering administration should cover sterilized method, makeup, safety checks, and documentation.
Adjuvants such as antiemetics, antispasmodics, and neuropathic representatives are the distinction between chasing pain and controlling it. Tiny information aid. A very early dose of ondansetron usually stops the cycle of vomit, missed analgesic, increased pain, and further opioid need.
Safety internet and edge cases
Two populations will certainly examine your training: older adults and those with substance usage disorders.
Older grownups have reduced physiologic reserves and multiple drugs. Renal function might be low also if creatinine looks regular. Start with non-pharmacologic actions and paracetamol if proper, short-term pain management courses stay clear of long-acting opioids, and display for ecstasy. I have viewed a neighbor's hip crack individual drift into confusion after what felt like a conventional opioid dosage. The resolution was time, fluids, family presence, and a cautious button to arranged non-opioid analgesics.
Patients with opioid resistance or a history of misuse need clear, compassionate care. Do not conflate under-treated pain with drug-seeking habits. Validate background, make use of objective searchings for, and communicate a plan. Short-acting, titratable opioids with close tracking are commonly safer than high initial dosages or long-acting formulations. Engage addiction medication early if readily available. Your documentation needs to show analysis, rationale, and agreements made.
Other side situations include maternity, where NSAIDs are commonly limited in the third trimester, and using nitrous or methoxyflurane calls for obstetric input. Asthmatics might not tolerate certain NSAIDs. Head injuries should have unique caution with sedating analgesics that shadow neuro checks. PUAEME008 training should prompt you to consider these threats prior to you draw up a syringe.
How programs analyze abilities, not simply knowledge
Most discomfort administration training courses for nurses that map to PUAEME008 make use of a blended format. Anticipate pre-reading on pharmacology, multiple-choice knowledge checks, and, most importantly, scenario-based evaluations. You might take care of a mock compound crack on a manikin, overview a standard patient with breathed in analgesia, or run a situation of severe stomach discomfort with advancing vitals. Assessors see your sequencing, interaction, and documents. Time stress is part of the layout. That is proper, considering that the system targets emergency situation pain management.
A fair program also includes debriefs that compare various risk-free approaches. As an example, one candidate might choose fentanyl titration after inhaled analgesia, another may prioritize a local block if a clinician exists to sustain it. Both can be right if the thinking and surveillance are audio. Excellent facilitators do not educate "one best way," they teach a set of safe options matched to context.
Documenting discomfort like a professional
If a case mosts likely to examine or coronial testimonial, the top quality of your pain documentation will certainly be on screen. Right here is a concise pattern that has actually stood more than years in ED and pre-hospital setups:
- Record the standard pain rating with context: place, personality, radiation, causes, and feature. "Discomfort 8/10, sharp, best flank to groin, colicky, worse with activity, nausea present." Justify your strategy in one sentence. "Offered likely kidney colic, begin ketorolac if renal function allows, plus ondansetron, reassess 10 minutes, consider fentanyl titration." Document the medication, dosage, course, time, and simultaneous interventions like splinting or ice. Reassess at specified intervals. Tape both subjective discomfort scores and objective indications: face, protecting, heart rate, breathing rate, and useful examinations like ability to deep take a breath or move the limb. Note adverse impacts or absences thereof, any type of dose changes, and the handover or discharge plan, including cautions concerning driving, added doses, and red flags.
Your notes become part of your discomfort monitoring qualification at work. They reveal scientific maturity and shield you and your patient.
Choosing in between general and role-specific training
There is worth in both wide discomfort administration training and concentrated, role-specific courses. A general pain monitoring certification course builds pharmacology and evaluation skills that equate throughout settings: ED, wards, aged treatment, and area. Role-specific PUAEME008 supply discomfort monitoring courses focus on emergency situation procedures, standing orders, and the logistics of analgesia in less regulated environments.
If you divided your time between ED triage and ambulance support, take the role-specific course initially. If you are early in your job or returning from a leave, begin with a wider discomfort management certification program to refresh fundamentals, after that add PUAEME008 for scope.
Pain management training courses for physiotherapists likewise exist, commonly highlighting non-pharmacologic techniques, placing, and graded exposure for chronic discomfort. Interdisciplinary sessions where nurses and physiotherapists train together can be eye-opening. You see how language and movement can decrease discomfort scores without a single milligram of medication.
Common challenges and how to stay clear of them
Three mistakes come up continuously in audit conferences. The initial is under-treatment because of be afraid of opioids or a lack of confidence. Patients remember when their discomfort is dismissed. If your evaluation sustains it, deal with early with risk-free representatives, display closely, and record the plan.
The secondly is over-reliance on a solitary medicine, specifically opioids. Balanced analgesia is usually far better. Combining paracetamol and an NSAID, including ice or splinting, and making use of antiemetics lowers the total opioid need and side effects. Assume in combinations.

The third is bad interaction. If you titrate analgesia, your associates need to know what you have done and just how the individual reacted. Handovers that consist of the trajectory of pain and feature assist the next team continue safely. "Discomfort from 9 to 6 after 50 mcg fentanyl, able to lie still for CT, respiratory system price secure at 16, plan even more 25 to 50 mcg if pain rises over 7, take into consideration ketamine if additional boluses needed."
Turning proficiency into habit
Competency is awarded on a date, yet skill grows with time. Develop 3 habits to keep your PUAEME008 sharp:
- Treat discomfort as a crucial indication plus a story. Ask the person what a successful outcome resembles. For some, it is resting without waking; for others, it is walking to the bathroom. Audit yourself. Once a month, evaluate a handful of your situations for time to initial analgesia, total doses, negative effects, and client remarks. Patterns emerge. You will certainly see where you regularly under-dose or overuse an agent. Rehearse the side instances. If your service allows it, run tabletop drills: extreme burns with restricted IV access, senior hip crack with ecstasy, pediatric crack with stressed parents. Self-confidence expands when you practice outside of crises.
Where PUAEME008 fits within wider expert growth
A pain management qualification is one rung on a ladder. After you master it, think about expanding right into sedation proficiencies, injury treatment, or regional anesthetic in partnership with medical colleagues. The material you learn below likewise improves chronic discomfort discussions. Individuals notice when a registered nurse clarifies why paracetamol and an NSAID, taken on routine, will assist them move in physio tomorrow, and how movement feeds back to reduce pain. That is the professional loophole that decreases readmissions and improves satisfaction.
For managers, sustaining discomfort management training for registered nurses is a safety and security investment. When personnel can evaluate and deal with early, time to imaging reduces, procedures go smoothly, and issues regarding being disregarded decline. A well-structured provide discomfort monitoring program additionally creates a common language across changes and self-controls. You will certainly hear it in handovers.
Final thoughts from the floor
I have given analgesia in a well-lit resus bay with full surveillance and in a roadside ditch with rain blowing sideways. The concepts did not transform. Analyze first, suit drug to device and danger, titrate with intent, and communicate the plan. PUAEME008 defines those habits and gives you the legal and professional scaffolding to act decisively.
If you are considering pain management qualification, choose a supplier that maps cleanly to the device, pushes you in practical circumstances, and provides functional responses. If you currently hold the credential, keep utilizing it purposely. Discomfort is complicated. Patients remember that took it seriously, and your skill can be the distinction between a distressing memory and a manageable one.